- Home
- Parents Home
- Allergy Center
- Asthma Center
- Cancer Center
- Diabetes Center
- A to Z Dictionary
- Emotions & Behavior
- First Aid & Safety
- Food Allergy Center
- General Health
- Growth & Development
- Flu Center
- Heart Health
- Homework Help Center
- Infections
- Diseases & Conditions
- Nutrition & Fitness Center
- Play & Learn Center
- School & Family Life
- Pregnancy Center
- Newborn Center
- Q&A
- Recipes
- Sports Medicine Center
- Doctors & Hospitals
- Videos
- Para Padres
- Home
- Kids Home
- Asthma Center
- Cancer Center
- Movies & More
- Diabetes Center
- Getting Help
- Feelings
- Puberty & Growing Up
- Health Problems of Grown-Ups
- Health Problems
- Homework Center
- How the Body Works
- Illnesses & Injuries
- Nutrition & Fitness Center
- Recipes & Cooking
- Staying Healthy
- Stay Safe Center
- Relax & Unwind Center
- Q&A
- Heart Center
- Videos
- Staying Safe
- Kids' Medical Dictionary
- Para Niños
- Home
- Teens Home
- Asthma Center
- Be Your Best Self Center
- Cancer Center
- Diabetes Center
- Diseases & Conditions
- Drugs & Alcohol
- Expert Answers (Q&A)
- Flu Center
- Homework Help Center
- Infections
- Managing Your Medical Care
- Managing Your Weight
- Nutrition & Fitness Center
- Recipes
- Safety & First Aid
- School & Work
- Sexual Health
- Sports Center
- Stress & Coping Center
- Videos
- Your Body
- Your Mind
- Para Adolescentes
Surgery for Tear Duct Blockage
What Is Tear Duct Blockage Surgery?
Doctors do tear duct blockage surgery to open a blocked tear duct. This brief outpatient surgery is done by an ophthalmologist (eye doctor). Kids usually go home the same day.
Why Is Tear Duct Blockage Surgery Done?
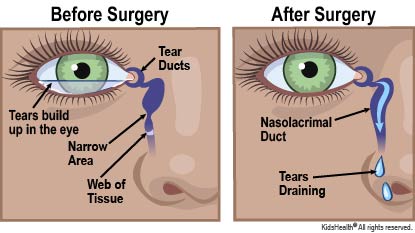
Tears need to drain out of the eyes. When a tear duct is blocked, the tears can't drain. Signs of a blocked tear duct include:
- too much tearing after a child is about 6–8 months old
- a serious infection of the tear duct
- infections of the tear duct that go away and come back again

30-Second Summary: Tear Duct Probe
Learn the basics in 30 seconds.
What Happens Before Tear Duct Blockage Surgery?
The ophthalmologist will do an eye exam to make sure your child has a blocked tear duct and not another eye problem that could cause similar symptoms. The doctor also might do a simple and painless dye test. Putting a special dye in the eye lets the doctor measure the amount of tears it makes and see if they're draining properly.
What Happens During Tear Duct Blockage Surgery?
Newborns sometimes can have a blocked duct opened in the ophthalmologist's office without anesthesia. Older infants and children need to go to a hospital or surgery center where they will get anesthesia (medicine to help them sleep and not feel pain).
An ophthalmologist can do different types of surgical procedures (sometimes in combination) to open a blockage:
- probing using a thin metal instrument: The ophthalmologist gently passes a thin metal instrument (probe) through the tear duct to open the blockage. Then they flush the duct with sterile water to make sure the pathway is clear. This is the procedure most often used for blocked tear ducts.
- silicone tube intubation: The ophthalmologist places silicone tubes in the tear ducts to stretch the ducts. The tubes stay in place for 3–6 months, then are removed either in the office or during another short procedure.
- balloon catheter dilation: The ophthalmologist puts a balloon into the tear duct and inflates it with a sterile solution. This expands the tear duct.
How Long Does Tear Duct Blockage Surgery Take?
The procedure takes about 10–20 minutes, depending on which type is done.
Are There Any Risks From Tear Duct Blockage Surgery?
Clearing a blocked tear duct is a very common and safe procedure. But all surgeries come with risks, including infection, bleeding, or problems with anesthesia.
Sometimes a tear duct can get blocked again and need another surgery to fix.
How Can Parents Help After Tear Duct Blockage Surgery?
Your child should have very little discomfort after the procedure. It's common for kids to have some bloody or pink-tinged tears and a mild bloody nose for the first 1–2 days after the procedure.
The doctor may prescribe eye drops after surgery and will tell you how to care for your child at home. Use the medicine exactly as directed. Babies and kids usually get better in about a week after surgery.
When Should I Call the Doctor?
Call the eye doctor if your child's eye is:
- red, swollen, or draining pus
- tearing for more than a week after surgery
If the tears look very bloody or your child has a lot of pain, call the eye doctor or go to the ER.

© 1995- The Nemours Foundation. KidsHealth® is a registered trademark of The Nemours Foundation. All rights reserved.
Images sourced by The Nemours Foundation and Getty Images.
