What Is an Ultrasound?
An ultrasound scan is a medical test that uses high-frequency sound waves to create live images from the inside the body. Also called a sonogram or sonography, ultrasounds let doctors see the body’s soft tissues, which X-rays can’t do.
Doctors order ultrasounds for many reasons, such as to look for the causes of pain, swelling, and infection. Ultrasound scans are safe and painless.
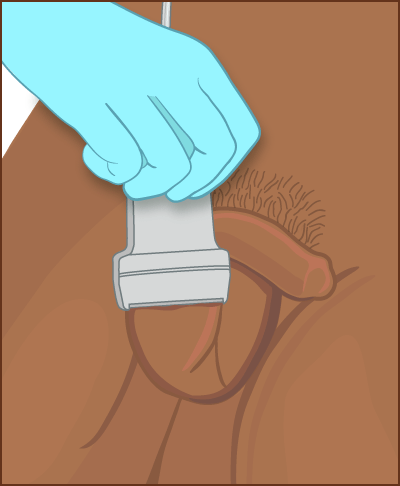
What Is a Scrotal Ultrasound?
A scrotal ultrasound test uses sound waves to make images of the scrotum (the pouch of skin at the base of the penis that contains the testicles). An ultrasound machine sends sound waves into the scrotum and images are recorded on a computer.
Why Are Scrotal Ultrasounds Done?
Doctors order a scrotal ultrasound when they're concerned about symptoms such as scrotal pain or swelling.
A scrotal ultrasound can show:
- the size of the testicles
- signs of injury to the testicles
- abnormally swollen veins in the scrotum (varicocele)
- fluid collection around the testicle (hydrocele)
- twisting of the testicle (testicular torsion)
- infection or inflammation in the epididymis (epidydimitis) or in the testicle (orchitis)
- a cyst or tumor in the scrotum
- an absent or undescended testicle
What if I Have Questions?
If you have questions about the scrotal ultrasound or what the test results mean, talk to your doctor.