Anterior Cruciate Ligament (ACL) Tears
What Is the Anterior Cruciate Ligament?
The anterior cruciate ligament (ACL) is one of the ligaments in the knee joint. A ligament is a tough, flexible band of tissue that holds bones and together.
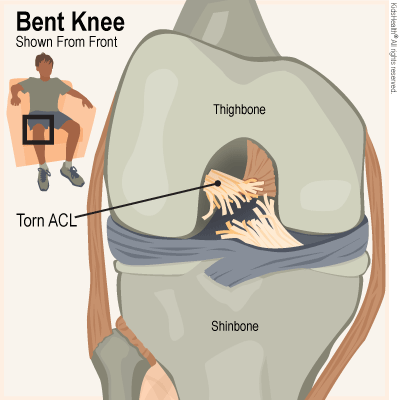
The ACL connects the bottom of the thighbone (femur) to the top of the shinbone (tibia). The ACL helps keep the knee stable.
What Is an ACL Tear?
The anterior cruciate (KROO-she-ate) ligament can tear if an injury stretches it too much. The tear might be partial (through a part of the ACL) or complete (all the way through the ACL).
What Are the Signs & Symptoms of an ACL Tear?
Most people who tear their ACL feel pain and a "pop" in their knee when the injury happens. Their knee usually gets swollen soon after the injury. After the swelling goes down, someone with an ACL tear usually can walk. But the knee may feel unstable and can "give way" and make the person stumble or fall.
What Causes ACL Tears?
Most ACL tears happen during athletic activity. For example when someone:
- changes direction or twists the knee while running
- jumps and lands in a way that twists the knee
The ACL also can tear if the knee is hit forcefully from the side.
Who Gets ACL Tears?
ACL tears happen most often during sports involving turning, cutting, and pivoting like skiing, soccer, football, basketball, and tennis. Women tear their ACL more often than men. This is most likely due to different anatomy.
How Is an Anterior Cruciate Ligament Tear Diagnosed?
To diagnose a torn ACL, health care providers ask about the injury and do a physical exam. During the exam, the health care provider presses on the knee and legs and moves them in certain ways. These tests can show if the ACL is torn.
Imaging tests that might be done include:
- X-rays to check for injuries to the bones
- an MRI to check the extent of an ACL tear and to see if the knee has other injuries
How Is an ACL Tear Treated?
Right after the injury, an ACL tear is treated with:
- RICE: Rest, Ice, Compression (with an elastic bandage), and Elevation (raising the knee)
- over-the-counter pain medicine such as acetaminophen (Tylenol or store brand) or ibuprofen (Advil, Motrin, or store brand)
Most partial tears can be treated with bracing and physical therapy (PT). A person might need to use crutches during recovery.
Some complete ACL tears will need surgery. Whether someone has surgery depends on many things, including:
- the type of the activities (or sports) the person wants to do
- if the person is an athlete
- age
- other injuries to the knee
- if the knee "gives way" or feels unstable
What Happens During Surgery for a Torn ACL?
ACL reconstruction surgery uses a graft (piece of tissue) to reconstruct (rebuild) the ACL. The graft can be a tendon, with or without bones attaching to it, from the patient's own body (called an autograft) or from someone else who donated the tendon (called an allograft).
ACL repair surgery is usually done arthroscopically. This type of surgery is done using a tiny camera (called an arthroscope) and small instruments that are inserted through small incisions (cuts).
Recovery from ACL surgery can take 6–12 months. A person may use crutches and a leg brace after surgery, and might need a knee brace after that.
Physical therapy is important to help the knee heal. PT helps to:
- improve range of motion and flexibility
- regain strength in the knee, thigh, and shin muscles
- reduce pain and swelling
- improve balance
How Can We Prevent Another ACL Tear?
Having an ACL tear puts someone at higher risk for another one. Training programs may help your child avoid another ACL tear. These focus on neuromuscular training (NMT). NMT teaches movement patterns that lower the risk of injury, especially while jumping, landing, and changing direction. NMT programs include stretching, plyometrics (jump training), and balance training.
Ask your care team if an NMT program is right for your child.
How Can Parents Help?
Recovering from an ACL tear takes time. It's normal for kids with ACL tears to feel angry, frustrated, or down, especially if they can't play a sport they love. Help your child find ways to stay involved in sports, such as keeping score or being a team manager. Or, if your child wants to do something besides sports, help him or her try a new hobby like playing the guitar, painting, or drawing.
To help your child get the best treatment possible:
- Go to all follow-up visits and physical therapy appointments as directed.
- Help your child follow the care team's instructions for at-home exercises.
