Kyphosis
What Is Kyphosis?
Kyphosis (kye-FOH-sis) makes a person's spine rounded so the back looks hunched over. Everyone has some rounding of the spine. But a larger rounding than normal can cause health problems like pain and breathing trouble.
Doctors sometimes treat kyphosis with back braces and physical therapy. A larger curve might need surgery.
What Happens in Kyphosis?
The spine is called “the backbone” but it's not just one bone. It's made of lots of small bones (called ) that are stacked and connected by a type of elastic tissue called cartilage. This gives us the flexibility to bend, stretch, balance, and walk.
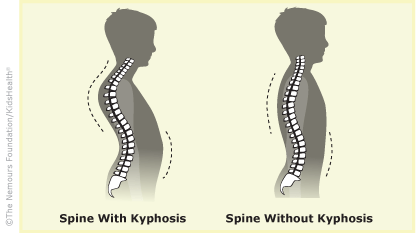
The stacked vertebrae are slight rounded, making the upper back curve out a little bit. When the curve is larger than normal, it's called kyphosis.
Kyphosis also can happen in the neck. This is called cervical kyphosis.
What Are the Types of Kyphosis?
The different types of kyphosis in the back are:
Congenital kyphosis: A problem with how the vertebrae developed before birth causes this type of kyphosis. It is more noticeable as a child grows.
- Read more about congenital kyphosis.
Postural kyphosis: This is the most common kind of kyphosis. Kids who slouch over a lot (have "bad" posture) can develop a rounded back.
- Read more about postural kyphosis.
Scheuermann's kyphosis: Viewed from the side, vertebrae look like stacked rectangles. In Scheuermann's kyphosis, the vertebrae are triangles, or wedge shaped. This makes the spine hunch forward.
- Read more about Scheuermann's kyphosis.
