What Is Torticollis?
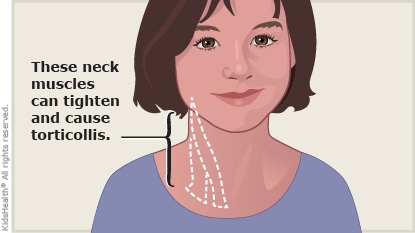
Torticollis (or twisted neck) means having a stiff and twisted neck that hurts. A twisted neck also makes the head tilt to the side.
Kids can develop torticollis (tor-tuh-KOL-is) for different reasons. The most common causes aren't serious. But sometimes a child with torticollis should see the doctor right away.
What Causes Torticollis?
Torticollis most commonly happens because of irritation to one of the neck muscles. This can happen when kids:
- sleep in a funny position, which stretches the neck muscles
- have a cold or throat infection, like mono or strep. The swollen that can happen with an infection can irritate the neck muscles.
Kids with muscle irritation triggering their torticollis often wake up from sleep with neck pain and stiffness.
Some kids can have torticollis from serious causes. The two most common are neck injuries or a retropharyngeal abscess. A child who has torticollis after an injury or has neck pain along with a fever and drooling or trouble swallowing should see a doctor right away.
Some babies are born with a different type of torticollis, which isn't painful.
What Are the Signs & Symptoms of Torticollis?
If your child's neck is painful to move, or if it feels tense or strained on one side, it could be torticollis. Another telltale sign: the head will tilt toward the sore side to relieve stress on the neck, and the chin will tilt in the opposite direction to relax the neck even more.
Kids with torticollis from irritated neck muscles also will feel pain when they turn the neck away from the side with sore, tight muscles or when they press on the sore area.
How Is Torticollis Treated?
How torticollis is treated depends on its cause.
Torticollis from irritated neck muscles usually goes away on its own. After a day of rest, a child's neck pain and head tilt should begin to go away, but might not be completely gone for a few days.
While the neck is getting better, have your child avoid straining it. To help your child feel better:
- Offer pain medicines like ibuprofen. If there is any muscle irritation, these can help heal the muscle as well as stop the pain.
- Use warm compresses over the part of the neck that hurts when moved. (If you use heat packs, never apply these directly to the skin. Instead, keep a towel or cloth between the heat and the skin.) Only use heat for 20 minutes at a time. You can apply warm compresses every 3–4 hours.
- If the pain does not ease with ibuprofen, the doctor may prescribe a medicine to relax the muscle for a few days.
Check your child's bed if they first complained of torticollis after waking up. A lumpy pillow or toys in the bed can create an uncomfortable night of sleep. (Remember, to help prevent SIDS, never let babies younger than 12 months old sleep with pillows, blankets, crib bumpers, or toys.) Making sure the sleep space is safe and comfortable may help the torticollis go — and stay — away.
Torticollis from an infection might need antibiotics to get better. If your child has a fever with torticollis, call your doctor.
Torticollis from a neck injury needs special care. Call the doctor or take your child for medical care if they have a stiff, twisted, or painful neck after an injury.
When Should I Call the Doctor?
If your child's neck pain doesn't get better after you provide home care and make their sleeping area more comfortable, talk to your doctor. Doctors diagnose torticollis by asking how the symptoms started (for example, after a sleepover party) and doing an exam. The doctor might order X-rays or other kinds of imaging tests.
Call the doctor or get medical care right away if your child has torticollis from a serious cause. Call 911 if your child fell or was injured and has a twisted neck.
Call the doctor if your child has a twisted or stiff neck or tilted head and:
- can't move the neck
- has a fever, headache, or sore throat, or is drooling
- has trouble swallowing, eating, or drinking
- complains of vision changes
- has recently started taking new medicines
- seems to be acting differently
If your child has a medical condition that affects the neck (like Down syndrome), call the doctor right away if your child complains of neck problems. If you're not sure if your child is at risk for neck problems because of a medical condition, call your doctor and ask.


